Advanced Fatty Liver Disease: Warning Signs to Know
Advanced fatty liver disease often develops quietly, with symptoms appearing only after meaningful liver damage has occurred. Many people assume...
Advanced fatty liver disease often develops quietly, with symptoms appearing only after meaningful liver damage has occurred. Many people assume feeling tired or bloated is “normal,” which can delay care. Understanding the advanced fatty liver signs highlighted below can help you recognize when something more serious may be going on and when to seek medical guidance. This article breaks down the most important warning signs, explains what they may mean, and offers practical, US-relevant next steps—without hype or fear-based claims.
What “Advanced” Fatty Liver Disease Really Means
As fatty liver disease progresses, the liver’s ability to function normally declines, which is when clearer symptoms tend to appear.
👉 Want to go further? Our complete breakdown of Early Signs of Chronic Kidney Disease You Should Know walks you through kidney health and function step by step.
NAFLD, NASH, and Cirrhosis—In Plain English
Fatty liver disease often starts as NAFLD (nonalcoholic fatty liver disease), where excess fat builds up in liver cells. In some people, it progresses to NASH, which includes inflammation and cell damage. Over years, this can lead to fibrosis (scarring). When scarring becomes extensive, it’s called cirrhosis. About 20–30% of people with NAFLD may progress to NASH, and a smaller percentage reach cirrhosis, often over 10–20 years.
👉 If you’re also working on topics related to equipment, our detailed guide on 10-Minute Core Burn Workout at Home (No Equipment) covers exactly what you need.
Why Symptoms Show Up Late
The liver has a remarkable ability to compensate. Even with significant damage, it may keep working well enough that you don’t notice problems. That’s why many advanced fatty liver signs—like jaundice or fluid buildup—tend to appear only after function is impaired. By the time symptoms are obvious, damage may already be moderate to severe, making early recognition especially important.
👉 This pairs well with our Body Warning Signs You Shouldn’t Ignore guide if you want the full picture on reading your body’s signals.
Key Warning Signs You Shouldn’t Ignore
Once liver function declines, several noticeable changes can occur throughout the body.
Unexplained Fatigue and Weakness
Persistent fatigue is one of the most common advanced fatty liver signs. This isn’t the usual end-of-day tiredness—it’s ongoing exhaustion that doesn’t improve with 7–8 hours of sleep. For example, people may feel worn out after light activities like walking a few blocks or doing household chores. Fatigue may be linked to altered metabolism, inflammation, and toxin buildup that the liver can’t process efficiently.
Jaundice, Dark Urine, and Pale Stools

As liver function worsens, bilirubin (a waste product) can build up. This may cause yellowing of the skin or eyes (jaundice). Urine may appear dark amber or tea-colored even when well hydrated, while stools may look pale or clay-colored instead of brown. These changes reflect disrupted bile flow and should prompt prompt medical evaluation, especially if they develop over days or weeks.
Abdominal and Fluid-Related Changes
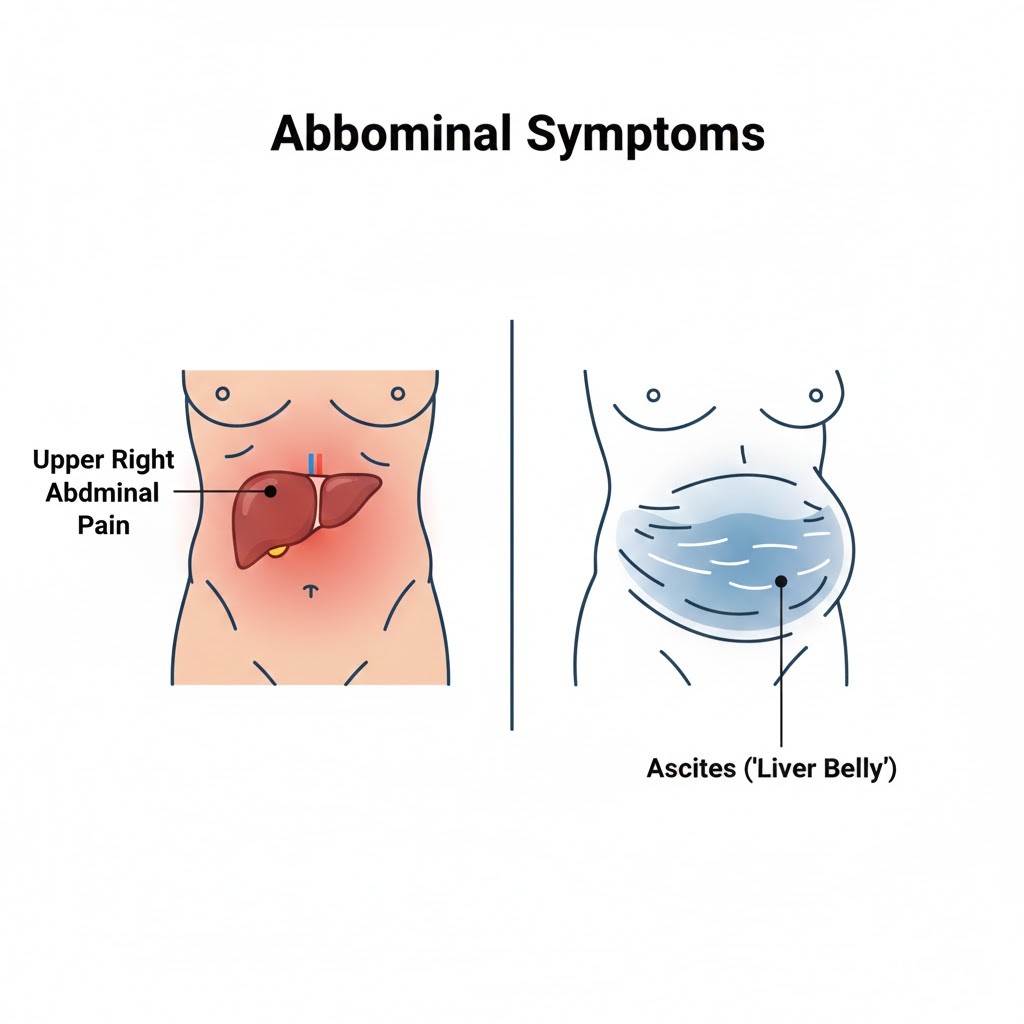
As damage advances, fluid balance in the body can shift in visible and uncomfortable ways.
Upper Right Abdominal Pain or Pressure
The liver sits under the right rib cage. In advanced disease, inflammation or enlargement can cause a dull ache or pressure in this area. It’s often described as discomfort rather than sharp pain and may worsen after large meals. For example, someone might notice fullness or soreness lasting several hours after eating a high-fat dinner.
Ascites and “Liver Belly”
Ascites refers to fluid buildup in the abdomen and is a hallmark advanced sign. The belly may look round or stretched and can increase in size over weeks. Even a 5–10 lb weight gain over a short period may be due to fluid, not fat. Ascites can make bending, breathing deeply, or tying shoes uncomfortable and typically requires medical management.
Swelling and Circulation-Related Signs
Liver damage can also affect blood flow and fluid regulation beyond the abdomen.
Leg, Ankle, and Foot Swelling
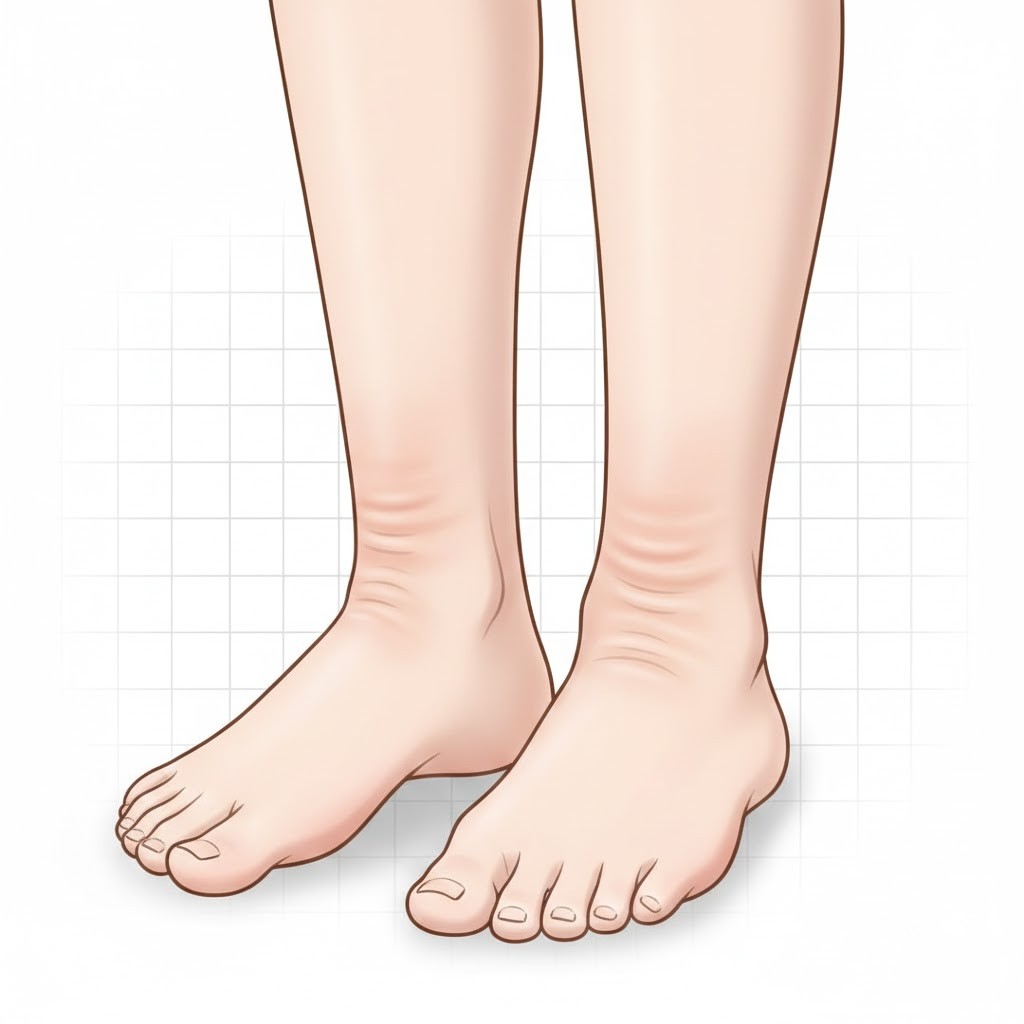
Swelling (edema) in the lower legs or ankles is common in advanced fatty liver disease. Shoes may feel tight by afternoon, or sock marks may linger for several minutes after removal. This happens when reduced liver protein production and altered blood flow allow fluid to leak into tissues. Swelling that worsens over days or extends up the calves deserves attention.
Easy Bruising, Itchy Skin, and Other Clues
People may notice bruises appearing after minor bumps or bleeding gums when brushing teeth. Chronic itching without a rash can also occur due to bile salt buildup in the skin. While each symptom alone can have other causes, a combination—such as itching plus swelling and fatigue—raises concern for advanced liver involvement.
When to See a Doctor and What to Expect
Knowing when to act can make a meaningful difference in outcomes.
Symptoms That Need Prompt Care
Schedule a same-week appointment if you notice persistent fatigue, abdominal swelling, leg edema, or color changes in urine or stool. Seek urgent care or call 911 for severe confusion, vomiting blood, black tarry stools, or sudden intense abdominal pain—these may signal complications of advanced liver disease.
How Doctors Evaluate the Liver
Evaluation often starts with blood tests like AST, ALT, bilirubin, and INR. Imaging such as ultrasound or FibroScan can estimate fat and scarring without surgery. In some cases, a biopsy is recommended to confirm severity. Tracking symptoms, weight changes, and medications beforehand can help make visits more productive.
Practical Steps That Support Liver Health
While medical care is essential, everyday habits still matter.
Food, Weight, and Lifestyle Basics
Many clinicians recommend a Mediterranean-style eating pattern emphasizing vegetables, beans, whole grains, fish, and olive oil. Even a 5–10% weight reduction has been associated with improved liver markers in some people. Aim for at least 150 minutes per week of moderate activity, like brisk walking, as tolerated.
Alcohol and Medication Safety
Avoiding alcohol is often advised once disease is advanced, even if alcohol wasn’t the original cause. Review over-the-counter meds and supplements with a clinician; for example, excessive acetaminophen (over 3,000 mg/day) can strain the liver. These steps don’t reverse disease but may help slow progression.
FAQs
1) Can advanced fatty liver disease be reversed?
Advanced fatty liver disease is difficult to fully reverse, especially once significant scarring has formed. However, progression can often be slowed. For example, losing about 5–10% of body weight, avoiding alcohol, and managing blood sugar or cholesterol may improve liver tests and symptoms in some people over time.
2) How long does it take for fatty liver to become advanced?
There’s no single timeline. In many cases, fatty liver progresses slowly over 10–20 years. Factors such as obesity, type 2 diabetes, poor diet, or regular alcohol use can speed up progression, while lifestyle changes and medical monitoring may slow or halt it.
3) Are advanced fatty liver signs always obvious?
No. Some people have advanced disease with only subtle symptoms like fatigue or mild swelling. Others develop more visible signs such as jaundice or ascites. Because symptoms can be mild or nonspecific, blood tests and imaging are often needed to assess severity accurately.
4) When should symptoms be treated as an emergency?
Get urgent medical care for severe confusion, intense abdominal pain, vomiting blood, or black, tarry stools. These may signal serious complications of advanced liver disease and should not wait for a routine doctor’s appointment.
If you recognize several advanced fatty liver signs in yourself or a loved one, don’t wait. Schedule a medical appointment, bring a symptom list, and ask clear questions. Early evaluation can help guide safer, more effective next steps.
Disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice.

About Jane Smith
We turn solid evidence into everyday habits Americans can actually do—plain English, cups/oz, grocery-aisle swaps, and routines that fit real life. Our editorial process: Experience—we road-test tips in real schedules…