What Your Pain Might Be Telling You
Pain is one of the clearest ways your body communicates that something needs attention. Even small aches can carry helpful...
Pain is one of the clearest ways your body communicates that something needs attention. Even small aches can carry helpful clues about lifestyle habits, nutrient gaps, or early imbalances. Many people in the US experience recurring pain without knowing what might be behind it. By learning how pain signals work and what common patterns can mean, you can better understand your body and make informed decisions about your well-being. This guide explains the most common pain signals, why they appear, and how to support your body with simple daily habits.
Why Your Body Sends Pain Signals
Before looking at specific discomforts, it helps to understand what pain signals actually represent. Pain isn’t random—it’s a messenger.
How pain can reflect lifestyle or nutrient gaps
Some pain signals are the result of everyday habits. Sitting at a desk for hours can tighten the shoulders and lower back. Not drinking enough water may lead to headaches or leg cramps. Up to 40% of adults in the US fall short on essential nutrients like magnesium, vitamin D, or B12. When these nutrients are low, the body may respond with symptoms such as muscle cramps, tingling, or fatigue.
For example, low vitamin D can contribute to knee or hip discomfort, especially during winter months when sunlight exposure decreases. Magnesium gaps may lead to night cramps that last 10–60 seconds. B12 shortages often show up as tingling fingers. These symptoms don’t provide a diagnosis, but they do offer valuable clues that your body may need more support.
When to take symptoms seriously
While some pain is linked to routine habits, other symptoms should be taken more seriously. Pain that keeps coming back, lasts for several days, or interrupts sleep may be a sign that something deeper is happening. Burning feet, for example, can appear in people with blood sugar imbalances. Sharp back pain combined with urinary changes might point to kidney irritation. Chest discomfort—even if you think it’s heartburn—should always be evaluated if it continues longer than a few minutes.
If pain worsens over time, comes with dizziness, numbness, or trouble breathing, or prevents normal daily movement, contacting a healthcare provider is important.
Common Pain Points and Possible Causes
Now that you understand why pain signals occur, let’s look at some of the most frequent patterns Americans experience and what they may indicate.
Joint and muscle pain patterns
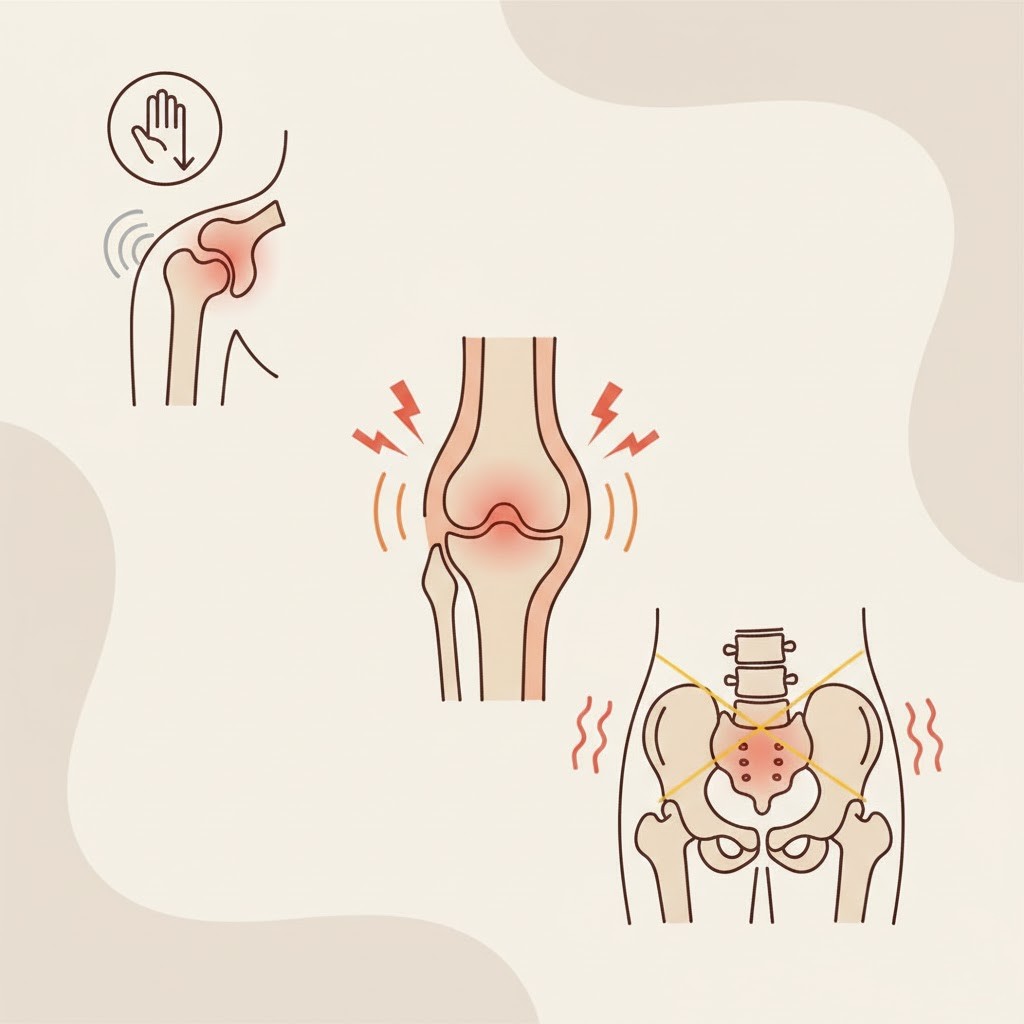
Joint and muscle pain often appear in areas that bear weight or remain still for long periods—such as the knees, shoulders, or lower back. Sitting for extended periods, lifting improperly, or repetitive movements can strain these areas. For example, knee discomfort may appear after standing for 30 minutes if the surrounding muscles are weak or tight. Shoulder tightness may follow long computer sessions or sleeping in an awkward position.
Some pain patterns may also be influenced by internal factors. Low vitamin D levels can contribute to knee soreness. Stress can tighten shoulder muscles, leading to tension headaches. Low back pain that feels deep or sharp may occasionally be linked to kidney irritation, especially when paired with urinary changes. Keeping track of when pain appears—such as first thing in the morning or after walking a mile—helps you recognize patterns and possible triggers.
Nerve-related discomfort and vitamin deficiencies
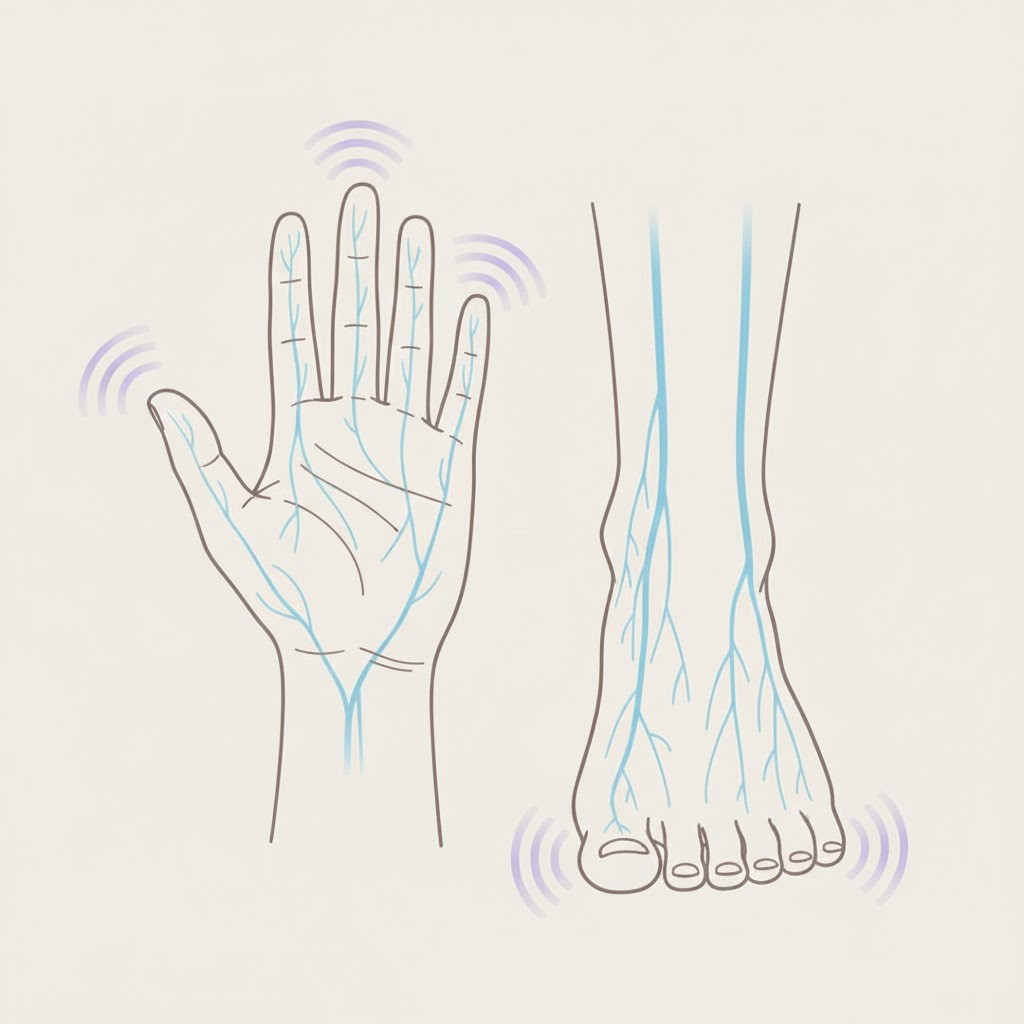
Nerve discomfort tends to be more specific. Tingling fingers, for example, can be connected to low vitamin B12 levels, which affect older adults more often. Burning sensations in the feet may be an early sign of blood sugar imbalance. Night leg cramps lasting 10–60 seconds may relate to low magnesium or dehydration.
Nerve-related pain often follows a clear path—down an arm, into the hands, or along the legs. These patterns help identify whether the discomfort comes from posture, nutrient gaps, or pressure on a nerve. While none of these symptoms confirm a diagnosis, they offer helpful starting points for conversations with your clinician.
When to Seek Professional Care
If you recognize any of the pain patterns above, the next step is knowing when to seek medical evaluation.
Red flags you shouldn’t ignore
Some pain signals require prompt attention. You should contact a healthcare provider if you experience:
-
Chest pain lasting more than a few minutes
-
Sudden numbness or weakness
-
Severe back pain with fever or changes in bladder control
-
Burning feet paired with increased thirst or fatigue
-
Pain that interrupts sleep multiple nights per week
These symptoms can indicate underlying conditions that need specialized care.
How doctors evaluate unexplained pain
Doctors typically begin with questions about your symptoms—how long they last, how often they appear, and what makes them better or worse. They may order blood tests to check vitamin D, B12, magnesium, blood sugar, or kidney markers. Imaging such as X-rays or ultrasounds may help identify structural issues.
Many clinicians recommend starting with simple lifestyle changes such as improving hydration (64 oz or more per day), increasing movement, or adding foods rich in essential nutrients. These first steps can reduce pain frequency and provide clearer insight into potential causes.
Simple Daily Habits to Support Overall Comfort
Once you know what your pain signals may represent, small daily habits can help reduce discomfort and support long-term wellness.
Diet and hydration basics
A balanced diet plays a role in how your body feels each day. Magnesium-rich foods—spinach, almonds, black beans—support muscle relaxation. Fatty fish like salmon and tuna supply omega-3s, which help maintain joint comfort. Drinking at least 64 oz (8 cups) of water daily supports muscle and nerve function. Even mild dehydration can trigger headaches or cramps.
Adding 2–3 servings of fruits and vegetables can boost your intake of vitamins and antioxidants that help your body respond better to stress and activity.
Movement, posture, and stress management

Movement keeps the body flexible and reduces stiffness. Taking a 5-minute stretch break every 45–60 minutes can ease shoulder and back tension from long sitting periods. Low-impact activities like walking or swimming improve circulation and help maintain joint comfort.
Stress can make pain signals stronger by tightening muscles and increasing inflammation. Relaxation techniques such as deep breathing, meditation, or going outside for 10 minutes of fresh air can ease the body’s stress response. Even changing sleep position—like placing a pillow between or under your knees—can significantly improve morning comfort.
FAQs
1. Can nutrient deficiencies really cause pain?
Yes. Low magnesium, vitamin D, or vitamin B12 may contribute to headaches, leg cramps, tingling, or muscle tightness. These don’t guarantee a diagnosis, but they offer clues worth checking if symptoms continue.
2. How do I know if burning feet are serious?
If burning feet appear often, worsen at night, or come with fatigue or increased thirst, it may be worth checking blood sugar levels. A healthcare provider can help determine the cause.
3. Is shoulder pain always related to the gallbladder?
No. Most shoulder pain comes from posture, stress, or muscle strain. Gallbladder-related pain usually happens on the right side and after eating heavy or fatty meals.
4. When should I worry about chest pain?
If chest pain lasts more than a few minutes or spreads to the arm, jaw, or back, you should seek medical evaluation. It’s always safer to get checked.
5. Are night leg cramps dangerous?
They’re usually not dangerous, but they can be uncomfortable. Cramps lasting 10–60 seconds may be linked to dehydration or low magnesium. Increasing fluids or checking nutrient levels may help.
If your body is sending repeated pain signals, start observing when and where they appear. Small daily changes can make a big difference—and a healthcare provider can guide you if symptoms continue.
Disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice.

About Jane Smith
We turn solid evidence into everyday habits Americans can actually do—plain English, cups/oz, grocery-aisle swaps, and routines that fit real life. Our editorial process: Experience—we road-test tips in real schedules…


